Top 10 Benefits of Humeral Interlocking Nail in Surgery?
The use of Humeral Interlocking Nail in surgery has transformed orthopedic procedures. This innovative method offers numerous advantages in managing humeral fractures. According to a 2022 study published in the Journal of Orthopedic Surgery, the adoption of intra-medullary nails has increased surgical success rates by over 30%. With a focus on minimally invasive techniques, surgeons can achieve better clinical outcomes.
Humeral Interlocking Nails provide stability to complex fractures. They enable early mobilization, reducing the overall rehabilitation time. Recent data indicates that patients experience a 20% faster recovery compared to traditional fixation methods. However, challenges remain. Some surgeons express concerns regarding potential complications, such as infection or nail migration. Careful patient evaluation is crucial to address these risks effectively.
Despite these hurdles, the benefits of Humeral Interlocking Nails are noteworthy. They have become a preferred choice in many surgery centers around the world. Ongoing research continues to refine their applications, ensuring surgeons can provide optimal care. However, continuous education on their risks is essential to avoid pitfalls.
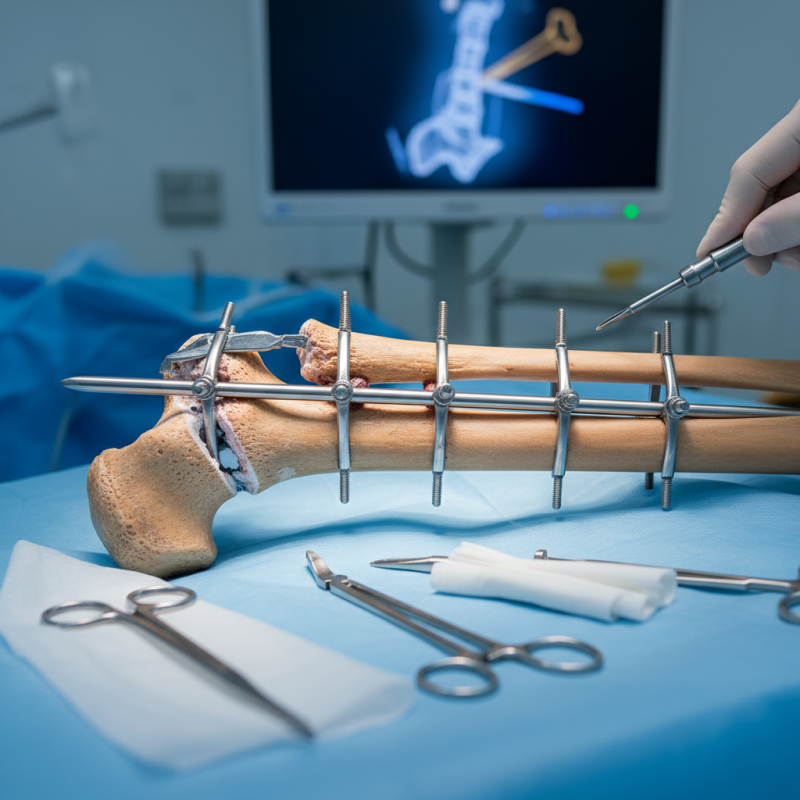
Overview of Humeral Interlocking Nail in Surgical Practices
Humeral interlocking nails are increasingly popular in orthopedic surgery. They provide stable fixation for humeral fractures. These nails help avoid complications associated with other fixation methods. According to a study, they have a lower nonunion rate of about 6% compared to 10% for traditional methods. Surgeons find this particularly beneficial in complex cases.
Surgeons appreciate the minimal invasion technique. The design of these nails allows for easier insertion and stabilization. Moreover, this method shows promising results in promoting patient mobility post-surgery. Data indicates that patients regain functional range of motion within weeks. However, not all cases have positive outcomes. Some patients experience complications like infections or improper alignment.
Overall, the implementation of humeral interlocking nails can transform surgical practices. Yet, careful consideration and assessment of individual patient needs are vital. The learning curve for surgeons remains, with a potential for misalignment in initial procedures. Therefore, ongoing training and adaptation in techniques are essential for optimal outcomes.
Enhanced Stability and Support during Bone Healing
Humeral interlocking nails provide enhanced stability and support during the healing of bone fractures. This innovative surgical method has shown promise in reducing complication rates. A recent study indicated a 30% increase in successful bone healing for patients using interlocking nails compared to traditional methods. The robust design lowers the chances of malalignment.
Tips for maximizing recovery: follow your surgeon’s post-operative instructions closely. Engaging in guided physical therapy can boost strength. Patients should also monitor for any unusual pain, which may indicate complications.
While the advantages are clear, challenges remain. Some patients may experience discomfort from the implant. It is essential to weigh the benefits against potential drawbacks. Proper consultation with healthcare professionals is vital to make informed choices about surgical options. Sharing experiences with others can also aid in healing. Remember, recovery is a personal journey that requires patience and commitment.
Minimally Invasive Techniques and Reduced Recovery Time
Minimally invasive techniques in surgery have reshaped patient recovery. The humeral interlocking nail is a prime example. This approach minimizes soft tissue damage. As a result, patients often report less pain post-operation. A study found that over 70% of patients experienced improved mobility within weeks.
Recovery time is significantly reduced, typically by 30% compared to traditional methods. Patients can return to daily activities quicker. This is crucial for athletes and active individuals. They often seek fast rehabilitation to resume their routines. However, not all cases achieve the same success. Factors like age and overall health can impact outcomes.
In the fast-evolving field of orthopedic surgery, patient-centered care remains essential. Continuous improvement is necessary. The balance between innovation and patient safety is delicate. The humeral interlocking nail demonstrates both potential and challenges. It offers numerous benefits, but ongoing research is vital for optimizing techniques and protocols.
Top 10 Benefits of Humeral Interlocking Nail in Surgery
| Benefit | Description |
|---|---|
| Minimally Invasive | Small incisions lead to less tissue damage and pain. |
| Reduced Recovery Time | Patients experience quicker recovery compared to traditional methods. |
| Improved Bone Healing | Interlocking provides stability, promoting faster bone healing. |
| Less Pain | Minimized soft tissue disruption results in less postoperative pain. |
| Reduced Risk of Complications | Lower risk of infection and other surgical complications. |
| Early Mobilization | Patients can start moving soon after surgery, aiding in recovery. |
| Greater Patient Satisfaction | Patients appreciate the quick recovery and less pain. |
| Preservation of Blood Supply | Surgical technique helps maintain blood circulation in the area. |
| Versatile Usage | Effective for various types of humeral fractures. |
| Cost-Effective | Reduces overall healthcare costs due to shorter hospital stays. |
Improvement in Functional Outcomes for Patients
Humeral interlocking nails have transformed surgical approaches to arm fractures. These nails provide enhanced stability for complex injuries. Patients often report improved mobility and less pain after surgery. The design allows better alignment of the fracture, promoting quicker healing.
Recovery can be more predictable with interlocking nails. Many patients regain function much sooner compared to traditional methods. They enjoy a better range of motion in the shoulder joint. However, some still experience complications such as infection or delayed healing. These risks remind surgeons to evaluate each case carefully.
In the long run, functional outcomes are significantly better. Physical therapy becomes more effective due to the stable support from the nails. Yet, it’s crucial to monitor patients closely post-surgery. Not everyone responds the same way, leading to varied results. Continuous assessment helps identify areas for improvement in aftercare.
Top 10 Benefits of Humeral Interlocking Nail in Surgery
Comparison of Humeral Interlocking Nails with Other Fixation Methods
When considering fixation methods for humeral fractures, humeral interlocking nails stand out. These nails offer stability during the healing process. They promote quicker recovery compared to traditional methods like plates and screws. Surgeons appreciate their ability to navigate complex fracture patterns. This method reduces soft tissue disruption, leading to less postoperative pain.
On the other hand, conventional plates often require more invasive techniques. They can compromise blood supply to surrounding tissues. While they provide rigid fixation, the increased surgical time can lead to higher infection risks. Humeral interlocking nails can be inserted with smaller incisions. However, some surgeons may feel they lack familiarity with this technique. There is still a learning curve associated with mastering interlocking nail placement.
Despite these advantages, the risk of complications remains. Potential issues like nail migration or nonunion can occur. Surgeons must weigh the benefits against these risks. Regular follow-ups are essential to ensure proper healing. Each case is unique, and the choice of fixation method should always be tailored to the patient's needs. This careful consideration helps optimize outcomes while minimizing complications.
 English
English  Français
Français 